Skin Care
Toothpaste on Pimple: Does It Work or Cause Harm? Dermatologist Explains
The remedy of applying toothpaste on pimples has been circulating for generations. Not to mention, most of us have tried toothpaste on pimple as a quick fix to dry it out overnight. We might think it is a good idea. Nevertheless, the truth is, toothpaste will do more harm than...
Skin Peeling On Hands: Causes, Treatments & Prevention
Our hands are constantly in use, regularly coming in contact with different things, chemicals, items, and applications, and are also always exposed to the elements in our environment. It is crucial to understand that the skin on our hands, just like any other part of our body, requires care and...
What’s True About Acne? Myths vs Facts Explained by Dermatologists
Though acne is a highly common skin concern, it is often neglected. People opt for home remedies to get rid of acne, believing they are safer and easier to use. These days, there is also a lot of misinformation easily available on the internet. Most of us fail to understand...
Skin Peeling On Face: Causes, Treatments, Home Remedies & Prevention
Are you worried about your peeling skin? Are you wondering what could be the reason behind the skin peeling on face and hands or anywhere else on the body? Well, skin peeling, also called skin desquamation, is usually the body’s healing response to certain skin ailments, medication side effects, or...
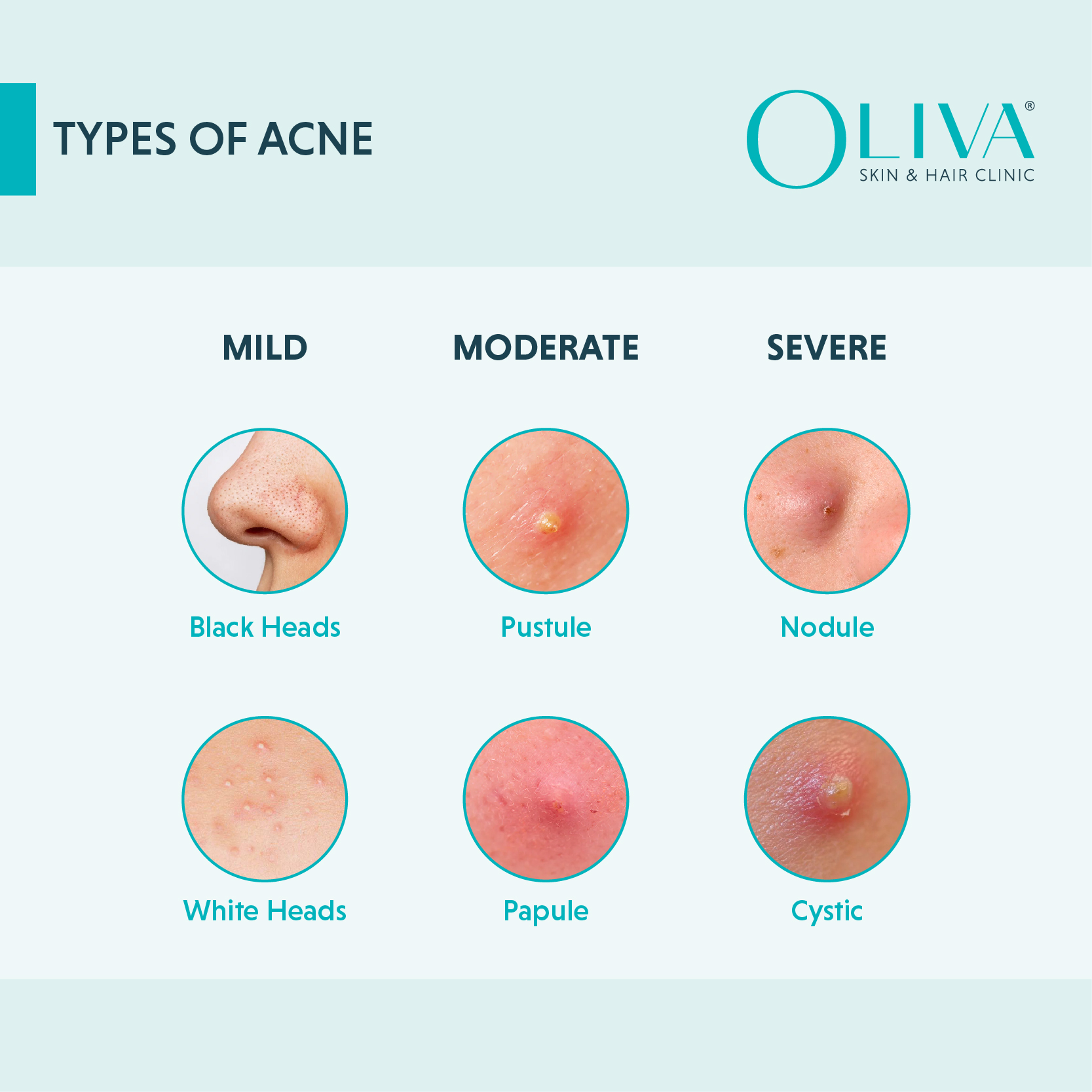
Different Types Of Acne: Causes, Symptoms, Treatments & Prevention
Acne is the most common skin concern prevalent in men and women of all ages. Most commonly seen in teenagers and young adults, due to hormonal fluctuations, acne can also occur during adulthood, especially in women. Acne, whose medical term is acne vulgaris, manifests in different forms, each with a...
Why Overnight Pimple Solutions Does Not Work?
Pimples or acne, as we know them, are a skin lesion with an acute inflammation brought about by certain factors such as excessive sebum production, pollution, dirt, hormonal imbalance, puberty, stress, lifestyle changes to name a few. Pimples affect mostly growing teens or those in their early twenties but there...
Laser Skin Resurfacing In Bangalore: Cost, Results & Procedure
If you are looking for a proven treatment to rejuvenate your dull, damaged, or ageing skin, you are on the right page. Laser skin resurfacing in Bangalore is one of the most advanced dermatological procedures that helps reduce wrinkles, scars, pigmentation, and other skin concerns, revealing clearer, firmer, and smoother...
Laser Hair Removal Aftercare: Tips For Better Results & Zero Side Effects
Laser Hair Removal (LHR) is the most advanced, scientifically proven, and safe dermatological solution for unwanted hair on all body areas. Concentrated beams of laser energy target and destroy unwanted hair follicles, reducing hair growth over time. [1] While the in-clinic procedure under the guidance of a dermatologist is simple...
Chemical Peel Treatment In Kolkata: Cost, Results & Procedure
If you're looking to reduce the appearance of acne, scarring, wrinkles, and sun damage to achieve clear skin, chemical peels might be your ally. Chemical peels in Kolkata are one of the most popular in-office treatments that address various skin concerns. Oliva Clinics has expert dermatologists who offer customised chemical...
Honey Benefits For Skin: Face Masks, Uses & Precautions Explained
Honey, the ancient beauty secret, is more than just a kitchen staple. For centuries, it has been cherished not only for its taste but also for its incredible healing and beautifying properties. Honey offers a myriad of benefits to the skin. From soothing irritation to fighting breakouts and boosting glow,...